
With labor costs and inflation going up—and not much help from reimbursement relief—in the HME industry, we find ourselves with further compressed margins. HME is reaching a point where modernizing your office and implementing better technology is a must-have for front- and back-office success. Understanding your workflow processes and systems matter.
To help providers, Joey Graham of Prochant and Ronda Buhrmester of the VGM Group came together on a webinar to walk through what it takes to optimize a healthcare intake team. An overview of the webinar is below.
What Is Intake?
Sometimes called the front office, intake includes these functions: your phone queue, fax wrangling, intake & eligibility, documentation, prior authorizations, and getting an order ready to be scheduled and dispatched.
The goal of intake is clean reimbursement. If your team can just get it right from the get-go, you wouldn’t need to go back and forth as much and could save time and money. Evaluating the processes you have in place can help.
Note: Front office means everything that happens before you fill the order. Back office is everything that happens after you fill the order—posting the cash, working in denials, and more.
Structure of Intake
Making sure you have the right staff is important for intake success and structure. Always hire based on your company’s core values. You can’t train skills or attitude, so take that into consideration when deciding who you will hire and train. Find the people who fit your company’s atmosphere, since you can train them in whatever area you put them in.
Smaller providers generally have one person or team to work as their customer service and handle front office functions. This one person/team does everything—answer the phone, grab the fax, enter the orders, check the eligibility, collect the money, and more.
However, as your company grows, you may have multiple teams split by function, branch, and payer. Your company structure depends on your payer and product mix, as well as your geographical reach. Consider these factors when trying to set your teams up for intake success.
Workflow with Systems
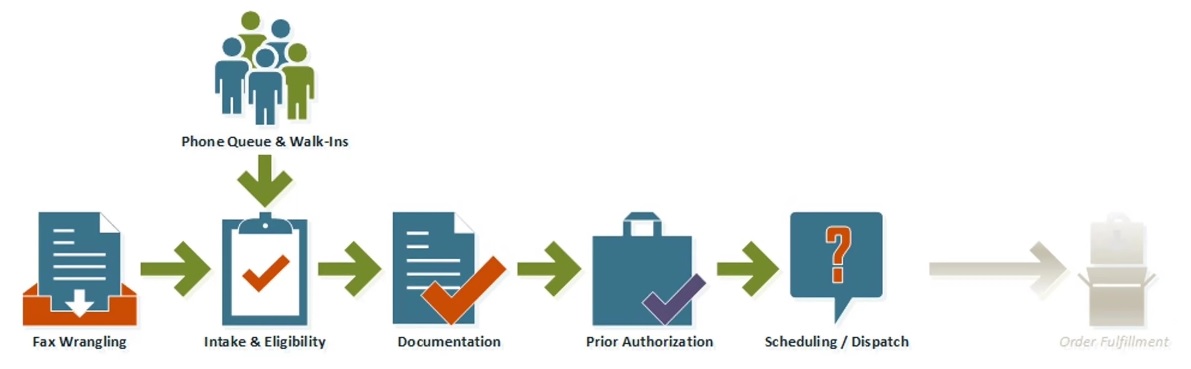
The vast majority of HME providers follow the below order of workflow. First, you start with managing your phone queue and walk-ins, people coming to your location. This leads to fax wrangling—incoming referrals. This is the person who is making sense of the authorizations and brand new orders.
With new orders, this leads to intake & eligibility—the person who is having to enter that patient and order, select the correct insurance, and make sure the insurance is eligible. If the intake & eligibility seems correct, it leads to the documentation step (i.e. to make sure the patient qualifies to get a ventilator). Then you can proceed to request authorization, if that’s required. Finally, you get the order over to your scheduling and dispatch team.
Understanding Your Systems
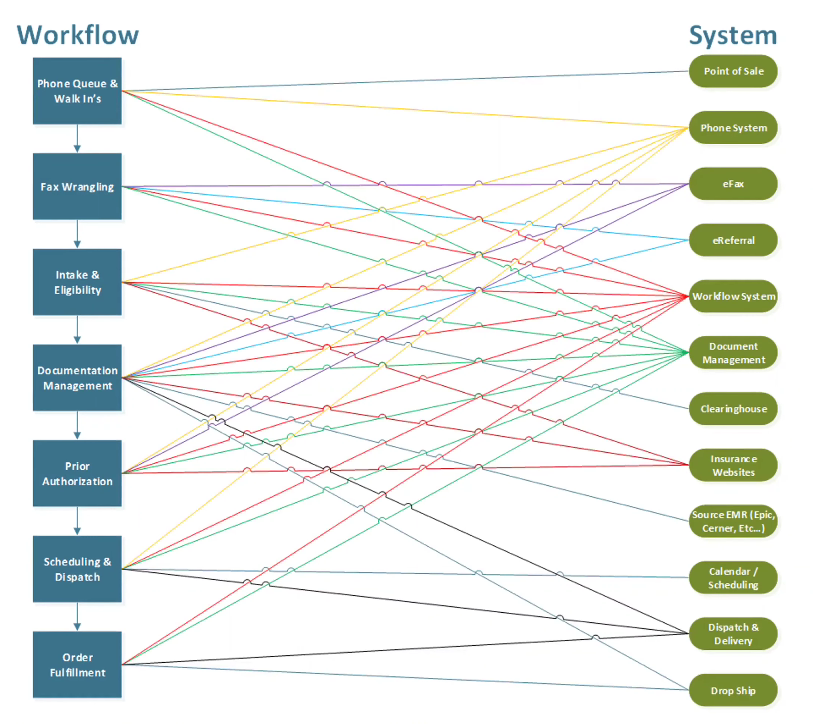
In the webinar, Joey talked through areas on the Workflow side of the graphic below and how they might interact with the System side. The system side includes your point of sale, phone system, eFax, eReferral, workflow system (billing system), document management, clearinghouse, insurance websites, source EMR, calendar & scheduling, dispatch & delivery, and drop ship.
In the graphic below, you have about 40 points of interaction between your workflow and systems. Every one of these interactions requires its own written procedure for how that system works.
Questions to Ask:
“How do we use these as a company?” Figure out what works best for you and your team(s).
“Who administers each system?” A lot of the time, whoever administered the system originally is no longer with the company.
“Are my systems supporting my processes?” Take time to reevaluate and find better alternatives.
“Do we have written standard operating procedures (SOPs)?” Written is the keyword here. Make sure SOPs are written. Tip: An easy way to do this is to, instead of wasting your time during work and typing processes in a document, conduct a Zoom meeting while you’re doing necessary processes and hit record on your screen. Go through each process while talking it through. Afterward, you will have that recording for whoever needs it and can also get a transcription of it.
To dive further into the workflow functions, we’ve broken down the functions by 1) which systems are involved and 2) the important questions to ask yourself or your intake team.
Phone Queues and Walk-Ins
The systems involved here are your point of sale and phone system.
Questions to ask:
- How do I match my products/services to my patient’s needs?
- Who is paying for it? (Do not ask this first.)
- Who is handling my walk-ins? Do they understand insurance coverage guidelines?
- How is the “retail” experience different from the “insurance” experience?
Tip: Try to separate your insurance staff and your retail staff. Ask yourself how you handle walk-ins and who on your staff understands the insurance coverage when there is a walk-in.
Fax Wrangling
On the systems side, this is your eFax and eReferrals, workflow/billing system, and documentation management.
Questions to ask:
- How do I route inbound documents/orders to my team?
- Is the patient picking up or is it being delivered?
- Did we acknowledge the order?
- Who oversees my billing/workflow system?
Intake & Eligibility
Systems included here are your workflow/billing system and documentation management, along with clearinghouse, insurance websites, and your phone system.
Questions to ask:
- What is the patient’s address? Do they live in my service area?
- How does my company handle order qualification?
- How does my company handle eligibility?
- What am I missing that I need to fulfill this order?
- Who on my intake team is ready to help with walk-ins?
- Where can I automate?
Documentation
The systems included here are your eFax, eReferrals and traditional referrals, phone system, workflow/billing system, and documentation management.
Questions to ask:
- Have I figured out everything I’m missing so I can resolve it in one call?
- Do I have access to referral systems? Should I?
- How do I know if I have the documentation I need?
- How is my team organized? By referral? By pod? By payer?
Prior Authorization
Systems involved here are the insurance websites, your phone system, eFaxes, workflow/billing system, and documentation management.
Questions to ask:
- Does this payer require a prior authorization (PA)? What is needed for the PA?
- How long does the PA take to review and get a response for?
- How long is the PA good for? Is a re-authorization needed and when? How do I proactively manage this?
- How do I handle the initial authorization vs. re-authorization?
- Have I filed the approved PA letter in the patient’s electronic file?
Scheduling & Dispatch
Systems included here are your workflow/billing system, documentation management, along with your calendar & scheduling, phone system, dispatch & delivery (including mobile), and drop ship system.
Questions to ask:
- Is this for pickup or delivery? Is it in stock? Is there a common carrier?
- How is the electronic paperwork process handled?
- How do I handle ABNs and other important documents?
- How do I handle dispatching after hours or while on call?
Next Steps
How do you reach intake success? Structure your team for success. Based on the size of your company, order volume, geographical reach, and more, evaluate what processes are working and what may need to be re-evaluated.
Have an understanding of your workflow and systems and how they interact with each other. Also make sure your processes are written and recorded so that you or someone else can always reference back to them.
When reconfiguring your processes, ask all the tough questions. Don’t just outline the easy route where nothing ever goes wrong. Have written steps in place to know what your team needs to do to reach preferable results.
Watch and listen to the full webinar to optimize your intake team for success:
Get a complimentary reimbursement audit to understand your KPIs and how it compares to industry benchmarks.
Prochant is the only AI-driven reimbursement service provider in the home-based care industry. We deliver focused revenue cycle management (RCM) solutions to healthcare providers with 7 wholly-owned global delivery centers. Our expertise lies in providing end-to-end RCM for home-based care, infusion, and specialty pharmacies, consistently delivering exceptional results to some of the leading healthcare providers in the country. We harness specialized automation technology and deep industry knowledge to streamline the time-consuming and expensive reimbursement process. As a result, we help healthcare providers accelerate their collections, increase revenue, and reduce operational costs while managing risk. Prochant is HITRUST certified, the gold standard for HIPAA security. For more information, please visit prochant.com.
