
The HME industry has been changing for years, but the pandemic unfortunately helped push too many pain points to the forefront. Between staffing shortages and high turnover, rising labor costs, and many more issues, HME providers are struggling.
As the nation’s leading HME billing and process outsourcing company, Prochant’s mission is to help providers meet their financial goals with scalable solutions. Our Chief Revenue Officer Joey Graham is a self-proclaimed “child of the HME industry” and recently discussed where HME is overall in 2022 and broke down workflow management for providers.
Often times, these are the questions Joey hears from HME providers around the country:
- How do we do more with less (staffing, reimbursement, time)?
- How do we make sure our workflow is modern and meeting the needs of the business?
- Is there any opportunity for us to leverage technology for better workflow management?
As the pandemic helped show, “just because we’ve always done things a certain way, it doesn’t mean we should continue doing it that way. Providers are having to reevaluate their whole workflow system to reduce pains in the process,” Joey said.
When Prochant experts say they understand the ins and outs of the HME industry, they mean it. Joey is now the Chief Revenue Officer at Prochant, but he started right out of high school working at a local provider in Florida. He was a warehouse technician, scrubbing and testing the equipment, as well as filling the oxygen tanks. He was also a driver, on call 24-hours a day, working with patients and traveling into the middle of nowhere in a company van. From there, he was a CSR, file clerk, biller, collector, and then the general manager for a regional DME provider all before he got picked up by Brightree as a senior consultant. Now, he understands the world of various different types of providers, from multi-billion dollar corporations to single store providers.
We asked Joey to breakdown the common terms we use when discussing HME billing solutions:
When we say the revenue cycle and workflow management, what are we talking about?
A visual of the HME revenue cycle is below for reference. Beginning at the top right, it starts with an incoming referral, and then it works its way through the circle. 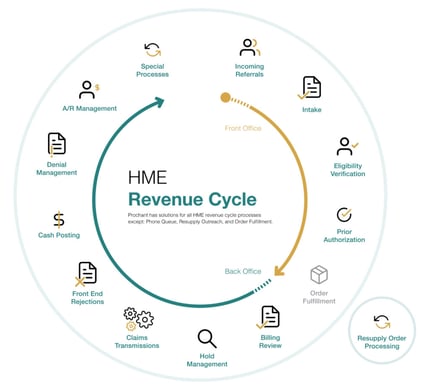
The front office is everything that happens prior to the product or service being provided to the patient. This includes incoming referrals, intake, eligibility verification, prior authorizations, and documentation review.
The back office is everything that happens after the product/service is provided to the patient, from order confirmation to claim resolution & closure. Back office includes order confirmation (billing review), hold management, front end rejections, cash posting, denials, and A/R management.
With workflow management, this is where we discuss with clients how their team is managing the flow of information through this revenue cycle circle.
Essentially, workflow management is about making sure every one of your referrals that comes in is tracked in some way and every order you fill gets billed and collected.
In our upcoming blog series on workflow management, we’ll be discussing traditional workflow management and the resulting problems, as well as technology and modern workflow management. Learn the differences from front-office vs. back-office workflow management and discover important things providers should be thinking about as they look to modernize their companies.
Looking for HME billing solutions now? Reach out to Joey directly at (980) 999-4293 or email joeyg@prochant.com to see how Prochant can help simplify your business.
Prochant has DME/HME clients from all over the country and handles front-end and back-end billing functions. Our scalable solutions, years of experience, and advanced technology provide best-in-class results to the healthcare community. Headquartered in Charlotte, North Carolina, our client base includes national HME and pharmacy providers and health systems.
